The claims
intelligence
system.
Purpose-built for auto PIP. Designed for a world where your models understand insurance, not just language.
Make claim intake
self-driving.
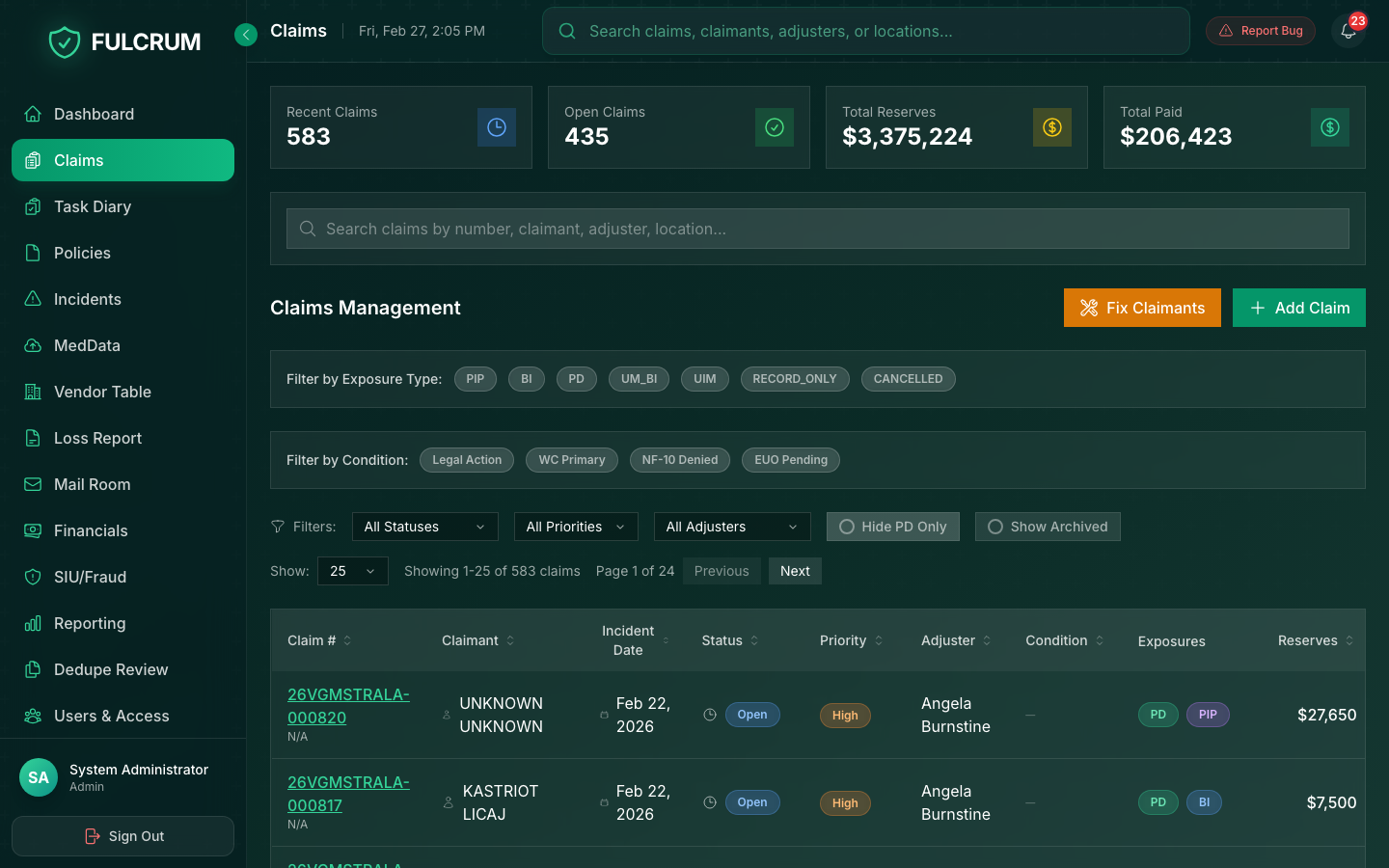
FNOL arrives — from a carrier portal, email, or API — and Fulcrum immediately captures structured data, validates coverage, assigns the right adjuster, and opens the file. No manual entry. No missed fields.
- Multi-channel FNOL ingestion (API, email, portal)
- Instant coverage verification & policy lookup
- Intelligent adjuster assignment by load & expertise
- Automated reserve calculation from FNOL data
Every decision,
AI-augmented.
Fulcrum's models surface what matters. Fraud signals. Billing anomalies. Subrogation opportunities. Recommended actions. All generated from our proprietary models — not generic LLMs.
- Fraud risk scoring on every claim
- Fee schedule anomaly detection
- AI-generated claim summaries & recommendations
- Resolution timeline prediction
Compliance,
automated.
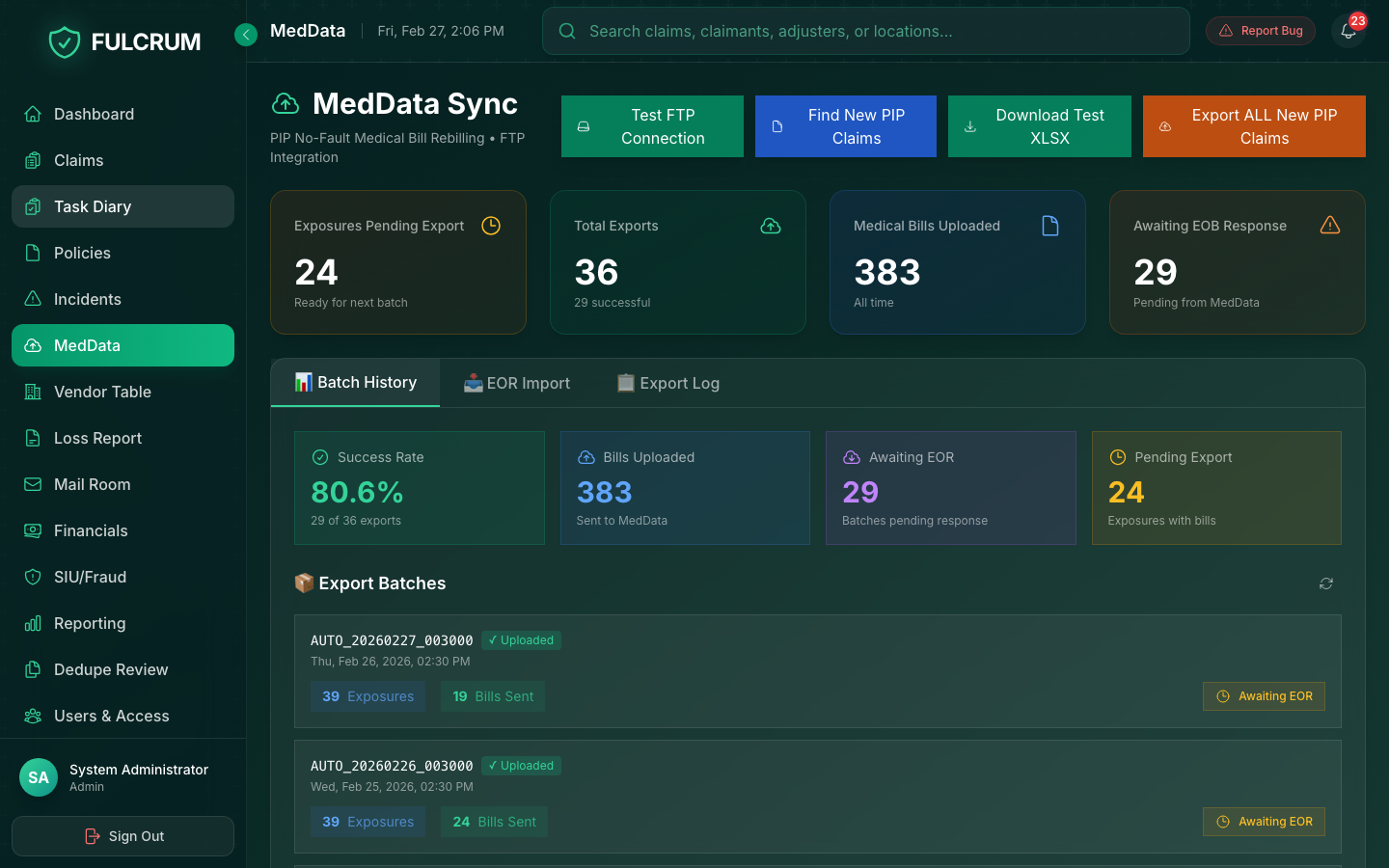
NY's 30-day PIP processing windows, NF-10 denial requirements, EUO tracking — Fulcrum handles the compliance layer so your team doesn't have to remember deadlines.
- Automated NF-10 denial generation & tracking
- IME request workflows with scheduling integration
- SLA deadline alerts before they breach
- Audit-ready documentation on every action
Understand your
book at a glance.
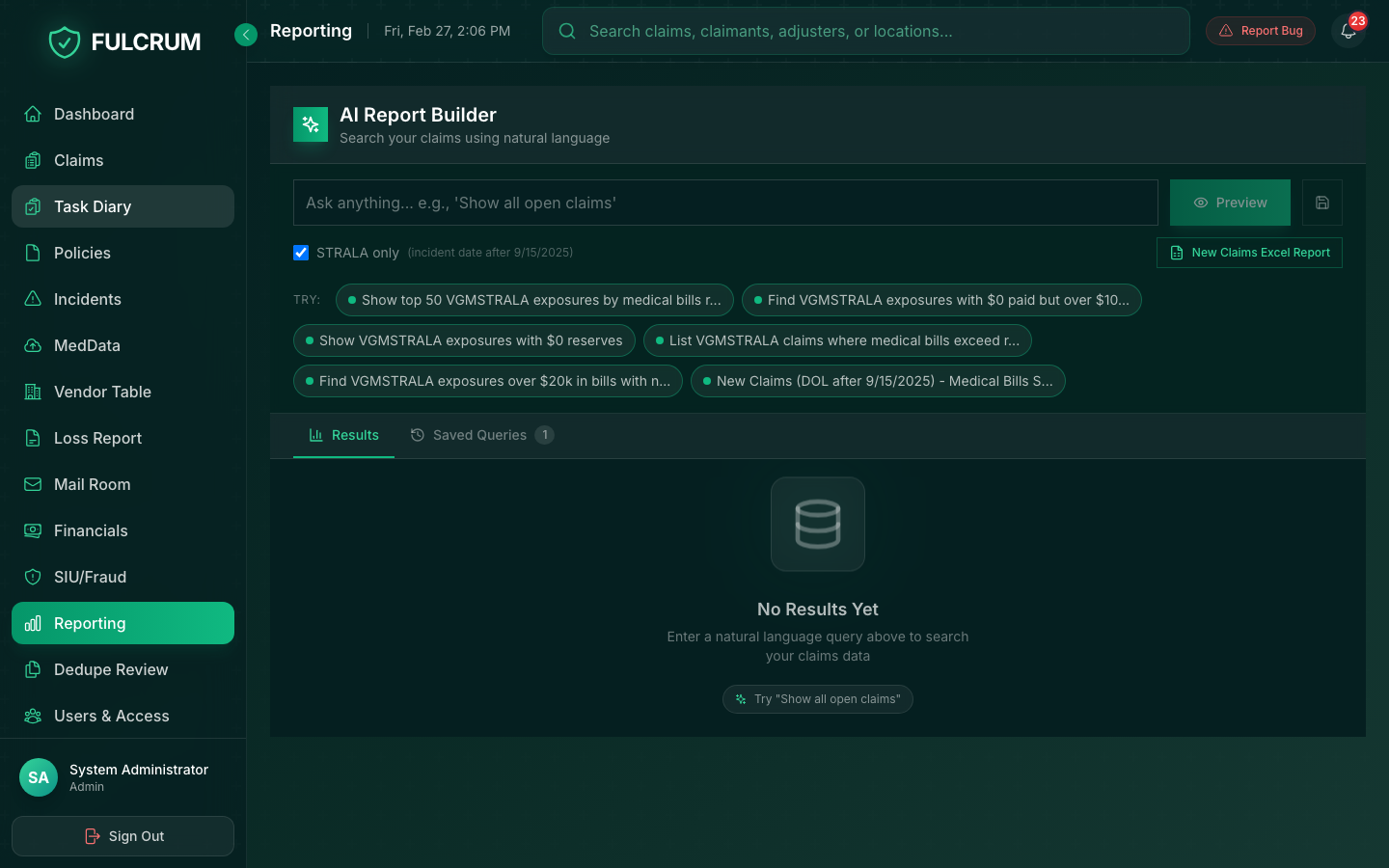
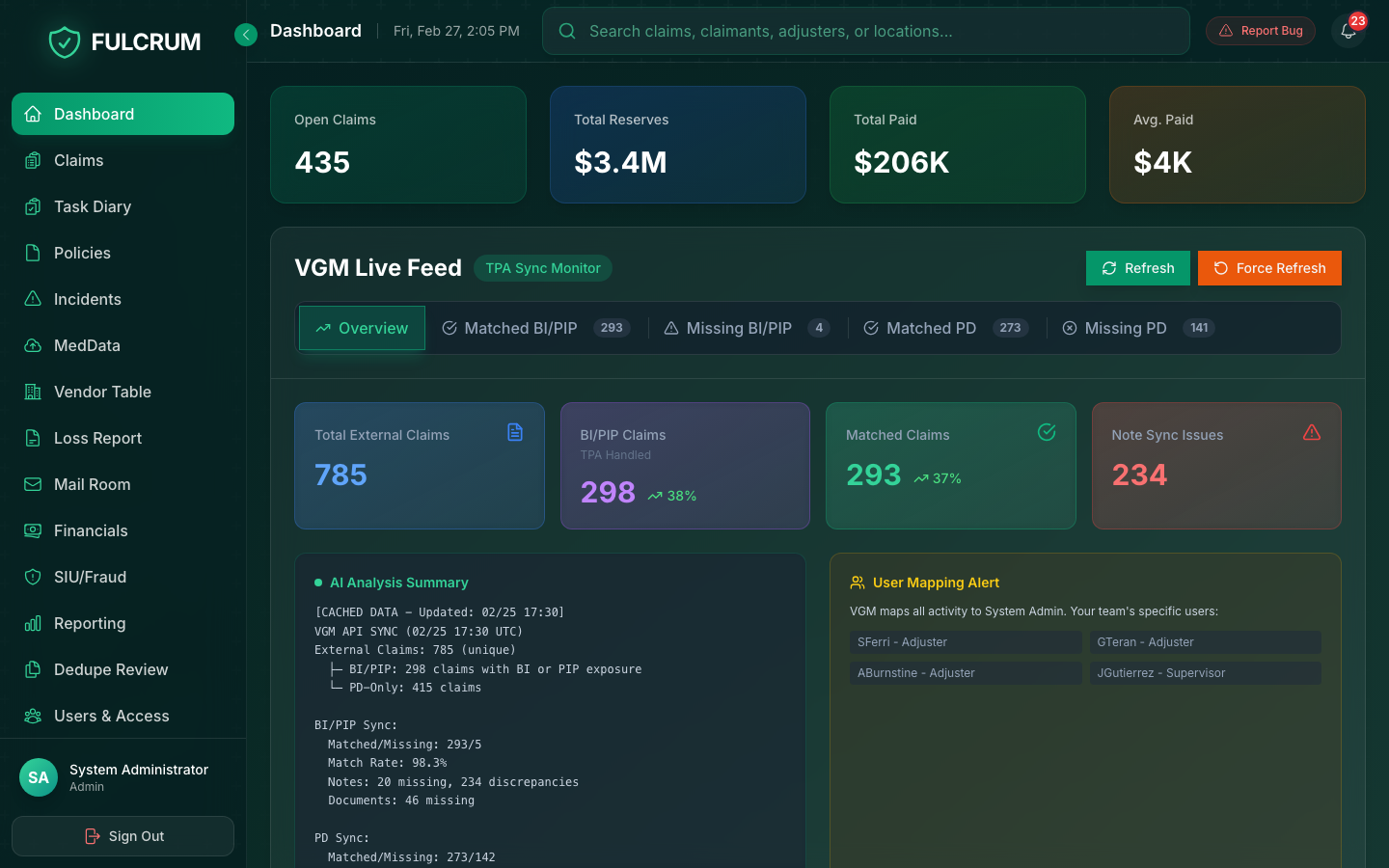
Real-time PIP dashboards, reserve trend analysis, and AI-generated insights give your leadership team the visibility to make decisions — not just reports to read.
- Live PIP intelligence dashboard
- Reserve trend & severity reporting
- AI-generated operational insights
- Custom report builder with natural language queries
We built our own models.
Because yours should
understand insurance.
Off-the-shelf LLMs don't know the difference between an NF-3 and an NF-10. They've never seen a NY PIP fraud ring pattern. Our models were trained on years of proprietary claims data — and they show it.
Document Intelligence
Trained on thousands of PIP forms — NF-2, NF-3, NF-10, EOR, IME reports. Classifies, extracts, and validates in seconds. 94% accuracy out of the box.
Fraud Detection
Pattern-matching against NY PIP fraud signatures — staged accidents, organized medical provider rings, inflated billing sequences. Surfaces signals human adjusters miss.
Medical Bill Review
Real-time NY fee schedule validation. Flags overbilled service codes, unusual treatment durations, and provider billing patterns before payment is issued.
Claim Summarization
Generates structured summaries of claim activity — coverage findings, treatment history, open actions — in the language insurance professionals actually use.
Subrogation Intelligence
Identifies subrogation opportunities at FNOL and throughout the claim lifecycle. Flags at-fault evidence, calculates recovery probability, and surfaces to adjusters before closure.
Outcome Prediction
Predicts claim resolution time, final reserve, and litigation probability from day one — giving your actuarial and underwriting teams the data they need, earlier.
Every claim processed on Fulcrum makes our models smarter. Outcome data, adjuster corrections, and fraud confirmations feed back into our training pipeline — creating a compounding advantage that grows with your book.
"NY no-fault is the most demanding auto claims environment in the country — strict timelines, aggressive fraud, among the highest litigation rates nationally. We chose Fulcrum because it was built to that standard from day one."